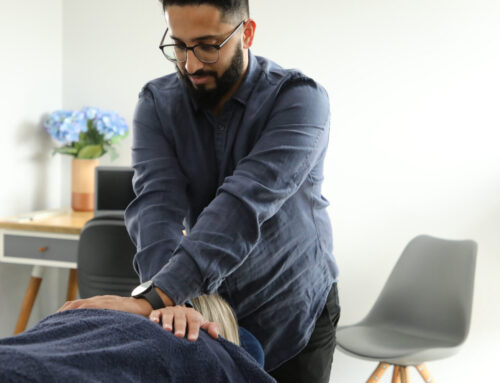
Approximately 90% of Australians will experience low back pain in their lifetime. With the numbers so high it’s no wonder it gets so much attention. However often people don’t manage it well due to the sheer volume of information – and not all of it is correct! There are a lot of unhelpful myths about what low back pain actually is and what we should do about it. This blog aims to debunk some of the common misconceptions about low back pain.
Myth 1: “I’m in heaps of pain so I must have really damaged my spine!”
As a general rule, there is little correlation between the intensity of back pain an individual is experiencing and the degree of tissue injury. Each individual’s experience of pain is unique and we all have different pain thresholds. Patients may report significant pain levels with minimal tissue damage, or alternatively feel very little discomfort with a severe injury. Often, patients experiencing very intense pain will have a significant decrease in their pain levels once their body understands it is no longer under threat.
Myth 2: “I should rest completely to let my back heal”
Whilst it may feel better to rest and do nothing, this can be one of the least beneficial things to do when experiencing back pain. In fact, prolonged sitting or immobility may worsen symptoms.
During acute back pain, it is best for you to keep mobile within pain free limits. This could include walking around the house every 20 minutes or simply changing positions frequently while you’re resting.
Recent studies are also showing exercise is an effective therapy for reducing chronic lower back pain and improving function.
Motion is lotion! It may help to improve healing, increase blood flow, lubricate joints and reduce muscular weakness associated with immobility.
Myth 3: “I need to get an Xray or scan to diagnose what is wrong”
Osteopath’s can typically develop a diagnosis based on the patient’s presentation so imaging is not always necessary. Imaging can be indicated when there is no improvement with treatment, to clarify the degree of injury or to rule out underlying conditions if suspected.
Commonly when patients undergo imaging, it reports very little significant findings relative to the patient’s back pain. Alternatively, some patients can experience no lower back pain but have incidental findings on imaging, for example, disc bulges.
Myth 4: “I should apply a heat pack to my back when it is painful”
For acute injuries, it is best to apply ice to the area of discomfort. As a general rule, do this for 10-20 minutes, 4 times per day within the first 24-48 hrs of injury. This acts as an anti-inflammatory measure, therefore may reduce pain and improve recovery.
Heat is generally more effective for chronic conditions that haven’t involved a specific injury, particularly muscular tightness. This helps increase the blood flow and nutrients to the area which may promote healing and reduce tightness.
Myth 5: “I have ‘put my back out’ and ‘need to see someone to put my back in’”
This is a very common myth! When our joints go “out” this refers to a dislocation which would indicate a medical emergency. More accurately, what is actually happening in an episode of back pain, is that a spinal joint become immobile. There are various causes for this including muscular strain or spasm, joint sprain or inflammation of the underlying tissues just to name a few.
Osteopaths work to release muscle tightness and improve joint mobility to relieve pain.
Hopefully this blog has shed light on some of the common misconceptions surrounding back pain. Should you be experiencing back pain or if you have any questions regarding this article, please email us on osteo@pakenhamosteopathy.com.au . We’d love to hear your feedback!
Thanks for reading!
Rebecca Kurrle (Osteopath)
Dreisinger, T. E. (2014). Exercise in the Management of Chronic Back Pain. The Ochsner Journal, 14(1), 101–107. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963038/